The NMPA – evaluating care processes and outcomes to identify good practice and areas for improvement
The National Maternity and Perinatal Audit (NMPA) is a large-scale audit of NHS maternity services across England, Scotland and Wales. Using high quality data, the NMPA evaluates a range of care processes and outcomes in order to benchmark against national standards and recommendations where these exist and to identify good practice and areas for improvement for women and babies. The audit is commissioned by the Healthcare Quality Improvement Partnership (HQIP) on behalf of NHS England and the Scottish and Welsh Governments. It consists of a continuous clinical audit, the first report of which was published in 2017, an organisational survey and a series of periodic audits on specific topics (‘sprint audits’).
Harriet AugheyClinical Fellow (Neonatal)
National Maternity and Perinatal Audit, Royal College of Obstetricians and Gynaecologists
nmpa@rcog.org.uk
The National Maternity and Perinatal Audit (NMPA) is a large-scale audit of NHS maternity services across England, Scotland and Wales. Using high quality data, the NMPA evaluates a range of care processes and outcomes in order to benchmark against national standards and recommendations where these exist and to identify good practice and areas for improvement for women and babies. The audit is commissioned by the Healthcare Quality Improvement Partnership (HQIP) on behalf of NHS England and the Scottish and Welsh Governments. It consists of a continuous clinical audit, the first report of which was published in 2017, an organisational survey and a series of periodic audits on specific topics (‘sprint audits’).
While the NMPA is primarily an audit of maternity services, it is also highly relevant to those providing neonatal care since the information made available by the NMPA relates to all mothers giving birth and, therefore, all babies born in Great Britain. This offers the opportunity to examine the wider context of these babies’ births: the settings they are born in, the characteristics of mothers and babies, and the events and outcomes affecting them. It also offers the opportunity to consider specific neonatal process and outcome measures and how these vary across maternity services.
The NMPA publishes information about the demographic characteristics of women giving birth in Britain. In the 2015/16 financial year, more than half of women giving birth were aged over 30 years, and less than half had a body mass index (BMI) within the normal range (FIGURE 1). These findings have implications for clinical outcomes, and for maternity and neonatal service provision.1
FIGURE 1 52.5% of women giving birth in 2015/16 were aged over 30 years and just 47% had a BMI within the normal range. These findings have implications for clinical outcomes and service provision.
Continuous clinical audit
The NMPA continuous clinical audit includes several measures relating to newborn babies, in particular five-minute Apgar score, skin-to-skin contact and breastfeeding. A five-minute Apgar score of <7 has been associated with an increased risk of cerebral palsy, epilepsy, developmental delay and infant mortality. Results suggest that 1.2% of singleton babies born at term in Britain have an Apgar score of <7 at five minutes of age. However, this proportion varies from 0.3% to 3.5% between maternity services despite adjustment for case mix (FIGURE 2).1
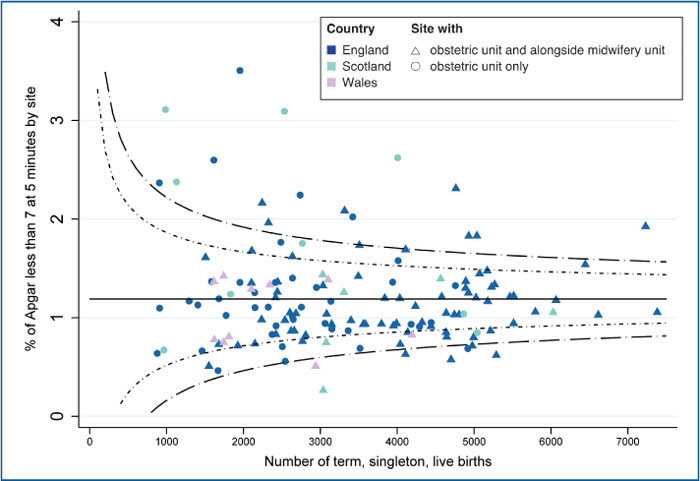
FIGURE 2 Site level proportions of singleton babies born at term who are assigned an Apgar score of <7 at five minutes of age, at sites with an obstetric unit.1
When looking at the proportion of term babies receiving skin-to-skin contact after birth and the proportion receiving breast milk at their first feed and at discharge, results show substantial variation in rates between providers. While this is likely to reflect true differences in practice between providers, it may also be the case that data entry for these variables is not always reliable. Measuring rates of skin-to-skin contact and breastfeeding is of great clinical relevance, since both are associated with improved outcomes for babies;2,3 through continuing to publish these data, the NMPA has a role in encouraging improved data recording, which can ultimately demonstrate improvements in care.
The full list of the NMPA measures is shown in FIGURE 3. Results published in the NMPA Clinical Report 20171 are available online at www.maternityaudit.org.uk, where they can be compared between sites or NHS trusts/health boards.

FIGURE 3 NMPA measures included in the first clinical audit report.
Organisational survey
The NMPA organisational survey provides a detailed snapshot of the configuration of maternity and neonatal services in England, Scotland and Wales at the start of 2017. This includes detail about levels of neonatal care available, the provision of transitional care and the availability of parent bedrooms on neonatal units. The survey found that maternity and neonatal services are organised in many different ways and ‘typical’ maternity units do not appear to exist. In addition, the configuration of maternity and neonatal services is subject to constant change, with many services reporting recent changes or changes planned for the near future.4
Sprint audit reports
As well as the continuous clinical audit and the organisational survey, the NMPA produces sprint audit reports on a series of specific topics. One of these is the neonatal sprint audit, which reports on the feasibility of linking the NMPA dataset with data relating to babies admitted to neonatal care. From this, additional neonatal-specific outcome measures will be produced as well as providing insights into the maternal antecedents of these neonatal outcomes. The second sprint audit considers maternal admissions to intensive care. Publication of both these reports is planned for early 2019.
Improving neonatal care is inextricably linked to improving maternity care. The NMPA offers an opportunity for neonatal and maternity service providers to use NMPA data collaboratively to identify areas for improvement and change. Working together to ensure the provision of high quality data within electronic systems ensures that results published are based on complete and robust figures, meaning subsequent service improvements can fully benefit the mothers and babies we care for.
Or read this article in our
Tablet/iPad edition


