Surfactant therapy – past, present and future
Surfactant replacement therapy for newborn infants with respiratory distress syndrome (RDS) has been available for about 35 years. During this time practice has evolved in relation to type of surfactant, timing and mode of administration. This review looks briefly at the history of surfactant use and how this has changed to shape current practice. We also speculate on potential future innovations that may further refine how this life-saving therapy is used.
Patrick M. McCrossanMB BCh BAO, MRCPCH
Paediatric Respiratory Fellow
Cystic Fibrosis Office, Great Ormond Street Hospital, London
mccrossp@tcd.ie
David G. Sweet
MD, FRCPCH
Consultant Neonatologist
Department of Neonatology, Royal Jubilee Maternity Hospital, Belfast
Respiratory distress syndrome
RDS, previously referred to as hyaline membrane disease, is primarily a disorder of surfactant deficiency resulting in pulmonary insufficiency developing soon after birth, mainly in preterm infants. The classical pattern of RDS has changed as treatments have evolved. X-ray appearances of ‘ground glass with air bronchograms’1 are rarely seen in the current era of antenatal steroids and early continuous positive airway pressure (CPAP) use. Definitions based on blood gas interpretation are also becoming redundant as clinicians have moved towards a more pragmatic approach of administering surfactant based on clinical assessment of work of breathing and inspired oxygen requirement very early in the course of the disease. As a result, more preterm infants are probably coded as having RDS on the basis that they have received surfactant treatment, which will give an overestimate of the true incidence. Without treatment infants with RDS may die, or spontaneous recovery occurs within 48-72 hours.
Endogenous surfactant
Pulmonary surfactant is a complex mixture of phospholipids and proteins produced by type II pneumocytes.2 Production begins from about 24 weeks’ gestation but only reaches full maturity close to term and the incidence of RDS is therefore inversely related to gestational age. Surfactant synthesis can be accelerated both by antenatal corticosteroids and perinatal lung inflammation in the setting of chorioamnionitis.3,4
The past
Discovery of surfactant
From as early as 1929 physiologists were aware of the presence of a substance in the lung enabling lowering of pulmonary surface tension. Animal experiments using nerve gases in the 1950s resulted in the discovery of bubbly lung fluid resistant to antifoaming agents and speculation that this was the substance lowering lung surface tension.5 Experiments on lungs of infants that died of RDS showed that the mean surface tension of these lungs was much higher than normal. It was concluded that: “RDS is associated with the absence or the late appearance of some substance which in the normal subject renders the internal surface capable of attaining a low surface tension when the lung volume is decreased.”6 The death of President Kennedy’s late preterm baby from RDS at two days of age increased public interest in the disease. Early trials with nebulised synthetic surfactant were not successful,7 however by 1973 studies involving preterm rabbits treated with natural surfactant showed positive effects on mortality.8 During this era, CPAP was being developed as a strategy to support breathing for infants with RDS, with some reported success.9
Surfactant trials in humans
The first human study using exogenous bovine surfactant was published in 1980. Ten preterm infants with severe RDS were given surfactant via an endotracheal tube. The infants responded with improved oxygenation and alveolar-arterial oxygen gradients, improvement in radiological findings and reduction in peak respiratory pressure.10 During the 1980s there was a dramatic increase in the numbers of clinical trials of surfactant, testing both synthetic surfactants (mixtures of phospholipids) and various animal derived natural surfactants. All of them showed clinical benefit, with reduced mortality, reduction of air leaks, but no overall impact on bronchopulmonary dysplasia (BPD).11 Further studies compared earlier versus later administration, as well as testing for differences among the various surfactant preparations.12-14 During this era, infants were typically managed in head box oxygen, then ventilated for a time after surfactant administration. Clinical trials convincingly demonstrated that giving surfactant prophylactically at birth improved outcome, reducing both mortality and air leaks, and during the late 1990s prophylactic surfactant administration became accepted best practice.
CPAP
Respiratory support using CPAP was developed during the 1970s, but fell out of favour as surfactant therapy gained precedence. CPAP can also prevent end expiratory alveolar collapse, reduce work of breathing and reduce ventilation-perfusion mismatch. It was observed that institutions maximising the use of CPAP had better respiratory outcomes,15 although it took considerable time before clinical trials would convincingly demonstrate that initiation of CPAP from birth was better than planning intubation for prophylactic surfactant. Animal studies show that even a very short period of manual ventilation can result in significant lung injury and this has potential to occur in infants undergoing early intubation.16 In 2008 the COIN trial (CPAP or intubation at birth), which included 610 preterm infants of 25-28 weeks’ gestation, offered reassurance that is was safe not to intubate immediately if the infant was supported with CPAP from birth.17 Cumulative data from clinical trials to determine whether prophylactic surfactant still conferred benefit if CPAP was used eventually showed that routine intubation for surfactant was potentially doing more harm than good.18
The present
Type of surfactant
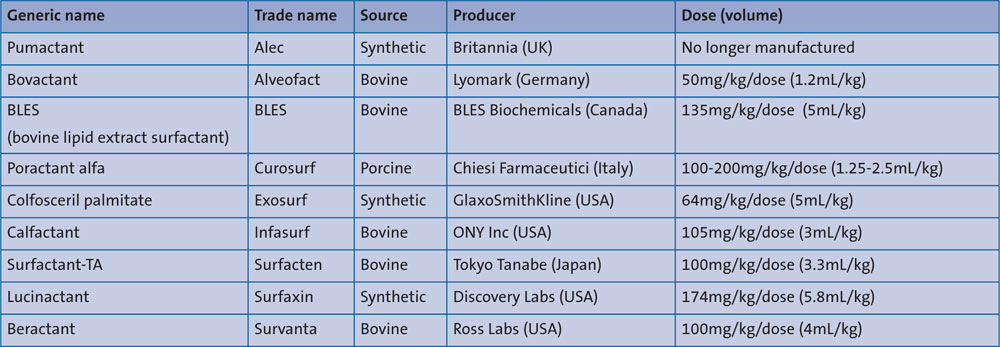
There are many types of surfactant with differing composition and dosing volumes available around the world (TABLE 1).19 During the 1990s clinical trials and meta-analyses of these trials convincingly demonstrated that animal derived surfactants were superior to synthetic surfactants which do not contain surfactant proteins. Natural surfactants have a more rapid onset of action and result in fewer pneumothoraces and reduced mortality.20 As a result, synthetic surfactants gradually disappeared from clinical use.
TABLE 1 Surfactant preparations and recommended doses.
Natural surfactants are typically derived from either bovine or porcine sources, and there are differences in surfactant concent-rations and dosage volumes among the various preparations available. A recent Cochrane review of 16 head-to-head trials comparing natural surfactant preparations has shown that there is little to choose between them in terms of clinical effect when used at the same dose, however for some preparations larger doses can be given resulting in better outcomes.21
Dose of surfactant
Surfactant pool size in healthy individuals is as low as 10mg/kg. Early animal studies showed clinical benefits of surfactant with doses as low as 20mg/kg. Later studies on human subjects used higher doses, decided pragmatically based on what volumes of surfactant would likely be tolerated, and these are the same doses that we use today, which vary among the various surfactants available (TABLE 1).
In the UK we only have access to poractant alfa or beractant. Poractant alfa is licensed for use at 100-200mg/kg. Studies of the pharmacokinetics of poractant alfa in infants show that the larger dose of 200mg/kg is associated with a longer half-life, with less need for additional surfactant dosing, fewer pneumothoraces and improved survival.21,22 It is thought that this difference is likely to be due to recycling of degraded surfactant components.23
Surfactant administration method
By 2013 it was accepted that surfactant prophylaxis, in the current era of prenatal steroid use, was no longer indicated for infants stabilised using non-invasive ventilation. A strategy of initiation of CPAP from birth with early selective surfactant administration for those showing signs of RDS was recommended. Traditionally surfactant has been given as an endotracheal bolus, followed by a short period of manual or mechanical ventilation, with subsequent weaning from ventilation as compliance improves. During the 1990s it was shown that surfactant can be administered followed by immediate extubation to CPAP, also known as the IN-SUR-E technique (INtubate- SURfactant- Extubate to CPAP).24 Meta-analysis of clinical trials of this method showed that ventilation can be avoided altogether in some cases, with an overall reduction in air leaks and BPD.25 Until recently this was considered the method of choice for spontaneously breathing infants with RDS, however in the last decade techniques have emerged for surfactant administration that theoretically can avoid exposure to positive pressure ventilation completely.
Two similar methods, both using a fine catheter that is positioned in the trachea while the infant remains on nasal CPAP have been developed.
LISA (less invasive surfactant administration) was developed in Germany.26 This technique involves placing a thin flexible catheter in the trachea using forceps with direct visualisation of the vocal cords via laryngoscopy. After catheter placement, the laryngoscope is removed and surfactant instilled intra-tracheally over 1-3 minutes during spontaneous respiration on CPAP. After instillation, the catheter is removed immediately.
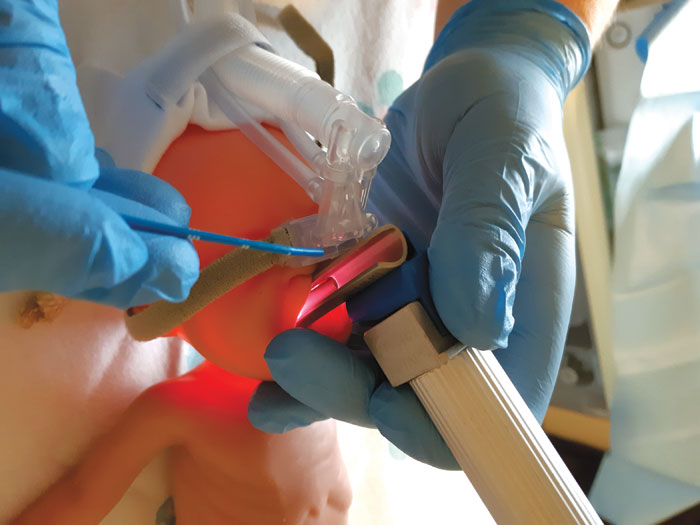
MIST (minimally invasive surfactant treatment) differs from LISA in that it employs a more rigid vascular catheter that can be placed manually (without the need for forceps) under direct vision (FIGURE 1).26 Both methods require laryngoscopy and the majority of clinical trials of these methods have not mandated sedation be used as maintenance of spontaneous breathing effort is paramount. Meta-analyses of studies using these methods show that ventilation can be avoided, and BPD can be reduced, and as a consequence the technique is gaining popularity around the world.27 Data from the German Neonatal Network has also shown sustained improvement in respiratory outcomes since widespread implementation of this method of early respiratory care.28
FIGURE 1 Training for minimally invasive surfactant administration. The infant is maintained spontaneously breathing on CPAP while a thin catheter is placed in the trachea using direct laryngoscopy. After placement of the catheter, the laryngoscope is removed then surfactant is administered slowly in small aliquots, as tolerated.
Timing of surfactant therapy
Infants at risk of developing RDS should be started on CPAP from birth. If they require intubation for stabilisation in the delivery room because of poor breathing effort or rapidly worsening respiratory status, they should receive surfactant as soon as correct placement of the endotracheal tube has been verified by auscultation and colorimetric carbon dioxide detection. If RDS develops more gradually, signified by increasing work of breathing and oxygen requirements, then a decision needs to be made about when to treat with surfactant. Surfactant, if required, works best if given earlier in the course of the disease.29 However, spontaneous recovery often occurs within 48-72 hours and avoiding exposure to any intubation if possible may reduce the risk of lung injury, creating a dilemma for clinicians. At present a reasonable threshold for intervention seems to be when the FiO2 (fraction of inspired oxygen) reaches 0.3 within two hours of age if the infant is worsening, as this is a reasonable predictor of later CPAP failure.30 For more mature infants this threshold may be higher.
The future
Alternative non-invasive surfactant administration strategies
The use of a laryngeal mask airway to administer surfactant may reduce the rate of intubation and mechanical ventilation for premature infants with moderate RDS. However, the size of laryngeal masks has limited use of this method to relatively mature preterm infants and routine use for infants most at risk is not yet recommended.31
Surfactant administered by nebulisation would be truly non-invasive and is theoretically plausible. However, lipids are notoriously difficult to atomise and traditional nebulisation methods have been unsuccessful.32 With the development of a new, customised vibrating membrane nebuliser, it has recently been shown that surfactant nebulisation can reduce the need for intubation in the first three days of life compared with nasal CPAP alone.33 However, these findings were limited to a group of patients at 320-33+6 weeks’ gestation and need to be confirmed with larger trials.
Bedside diagnosis of RDS
At present clinicians are limited to using inspired oxygen requirement, clinical assessment of severity of work of breathing along with radiographic findings in order to establish the severity of RDS. A rapid means of definitively diagnosing surfactant deficiency at birth would allow clinicians to predict those infants that would potentially derive benefit from early surfactant therapy.
Laboratory tests are available to examine the presence of endogenous surfactant from gastric aspirates. However, the complexity of these tests and the need for specialist training and equipment have precluded widespread introduction in to clinical use. Recently spectrometry has been used to measure the ratio of lecithin to sphingomyelin in gastric aspirates as a predictive test for RDS.34 This method could potentially be incorporated into a bedside analyser that could be used to determine if an infant requires early surfactant treatment.
New synthetic surfactants
Synthetic surfactants do not perform as well as natural, animal-derived surfactants because of the absence of surfactant proteins (SP-B and SP-C).19 Newer synthetic surfactants with the addition of protein analogues mimicking the effects of SP-B and SP-C have the potential to perform as well as, or better than, natural surfactants.35 They could be less expensive to manufacture and obviate the theoretical risks of immunogenicity or infection with the use of animal derived products.
Lucinactant, a protein analogue mimicking SP-B activity works better than protein-free synthetic surfactants and compared favourably to natural surfactants in clinical trials.36 Lucinactant requires special handling prior to administration and has a relatively high volume per dose, and therefore did not come in to wide-spread use and has since been withdrawn from the market. Other synthetic surfactants, such as CHF5633 containing both SP-B and SP-C analogues, are currently under evaluation in clinical trials.37
Surfactant as a vehicle for drugs
Surfactant combined with budesonide has been used in clinical trials as a means of preventing BPD. Two small studies from China have shown encouraging results, however more adequately powered trials with long-term follow up are needed before this treatment can be recommended.38 Perhaps in the future other drugs such as antimicrobials or antioxidants could be delivered in the same way.
Late surfactant
Traditionally surfactant replacement therapy has been limited to the first 48-72 hours of life as endogenous production begins shortly after birth. Recently two clinical trials have explored the effects of late surfactant administration for infants who remained stuck on mechanical ventilation beyond 1-2 weeks of age. A French study of 118 infants of <33 weeks’ gestation remaining ventilated at day 14 showed that surfactant therapy produced short-lived improvements in oxygenation, no significant reduction in BPD but significantly less respiratory morbidity reported by parents over the first year of life.39 A similar study from the USA randomised infants of <28 weeks’ gestation ventilated beyond day seven of life to inhaled nitric oxide plus repeated doses of surfactant, or inhaled nitric oxide alone. There was no reduction in BPD at 36 weeks’ corrected gestational age, however those receiving surfactant had less need for home respiratory support over the first year of life.40
Conclusion
Surfactant replacement therapy has revolutionised newborn care over the past quarter of a century. Ongoing research should further help to refine how and when to intervene with this life-saving treatment, and hopefully continue to result in improving longer-term respiratory outcomes for vulnerable babies that are born too soon.
Or read this article in our
Tablet/iPad edition
- During the 1990s it became common practice to routinely use ‘prophylactic’ surfactant in all infants below 30 weeks’ gestation.
- Continuous positive airway pressure (CPAP) from birth is also effective in managing RDS and thus creates a dilemma as to when to intervene with surfactant.
- Current practice is to minimise use of endotracheal ventilation by using less invasive methods for surfactant administration.
- Future improvements might include better synthetic surfactants, nebulised surfactant or the development of a bedside diagnostic test for early RDS.
Also published in Infant: