Speech and language therapy interventions for infants with feeding difficulties: considerations for service provision
Premature and medically fragile term infants receiving care on a neonatal unit are likely to have feeding difficulties. The provision of assessment and intervention from speech and language therapy (SLT) is vital as it improves short- and long-term feeding outcomes, which can reduce length of stay and improve quality of life for infants and their families. The anticipated investment in maternity services and a surge of funding for allied health professionals on neonatal units should improve service provision, including SLT, and have a positive impact on infant outcomes. This paper outlines the suck feeding journey and an ideal model of care for these infants, which focusses on improving neurodevelopmental outcomes.
Nicoll BellClinical Lead Speech and Language Therapist for Neonates, St George’s University Hospitals NHS Foundation Trust
nicoll.bell@nhs.net
Bell N. Speech and language therapy interventions for infants with feeding difficulties: considerations for service provision. Infant 2024; 20(1): 29-31.
Infants receive care on a neonatal unit (NNU) for a variety of reasons, prematurity being one. Length of stay on the unit depends on multiple factors including gestational age at birth, birth weight, sex, underlying medical conditions, dependence on respiratory devices and acquisition of suck feeding ability.1 Information about length of stay is essential because it can help with planning of service provision and provide timelines to parents at the start of their journey, which might bring some comfort at a stressful time.2
An infant’s feeding journey will progress on the NNU, with some achieving full suck feeding before discharge and others not. This will depend on underlying medical conditions, current gestational age, level of alertness in engaging with suck feeds and persisting respiratory illness, which might impact on the infant’s ability to successfully coordinate the suck-swallow-breathe (SSB) and feeding process.3 The ability to suck and swallow begins to develop in utero from 32 weeks’ gestation. This is a skill that will mature and after birth is paired together with breathing.3 An infant is required to suck, swallow and breathe in a harmonious cycle when suck feeding, which is a challenging task that may take weeks to master for some infants (often well post-term).3 Acquisition of suck feeding can frequently be the sole reason for a prolonged length of stay on a unit and may be the last milestone achieved before discharge is possible.1,4
When considering suck feeding acquisition, factors such as average postmenstrual age (PMA) at commencement and time to full suck feeds are important to note and can be offered as guidance to parents when their infant is starting the suck feeding journey.4-7 This is vital as feeding their child is a major event for parents on the unit; one that brings great reassurance. SLT can result in quicker acquisition of suck feeding skills in infants learning to feed on the NNU.6
This article will provide insight into the type of interventions infants should receive throughout their suck feeding acquisition journey, highlighting the need for specialist care from SLT. There has been a surge of funding in the UK for allied health professionals (AHPs), including speech and language therapists, on NNUs as a result of investment into maternity services following the Ockenden report.8 AHPs will be working towards meeting key performance indicators and looking to quantify the benefits of their interventions in order to secure further funding and, therefore, data that can be used to highlight the need for and benefit of AHP involvement are vital.
Infant feeding difficulties in the NNU
Data from a descriptive evaluation of early feeding development of infants in a local NNU indicate that a high majority of infants receiving care on an NNU, regardless of gestational age at birth, will have feeding difficulties.6 The retrospective data review found that the extremely preterm infant group is at significantly higher risk of poor feeding outcomes and begins suck feeding at a later gestational age, taking longer to achieve full suck feeding. This would be expected, given the greater complexity of their needs. The review also found that infants of any gestational birth age remain vulnerable and at risk of hospital re-admissions for some form of support post-discharge from the NNU.6
Neurodevelopmental interventions and SLT input
There are many neurodevelopmental interventions that can be implemented for infants on the NNU that will have benefits for feeding development. These include:
- positioning, eg swaddling, cuddling, nesting, containment, skin-to-skin/ kangaroo mother care or, at times, minimal handling
changes to the environment, eg reduction of stimuli, especially noise and light9
the introduction of pleasant stimuli, eg expressed breast milk (EBM) on a comforter placed near the infant
tactile interventions, eg positive touch or movement
auditory stimuli including the mother’s voice or music.9
Such general interventions are aimed at improving the infant’s experience and decreasing stress, which have been found to have a positive effect on growth and development.10 These interventions rely on a multidisciplinary approach that includes all clinical staff on the unit, particularly AHPs.
An infant’s feeding journey starts with pre-feeding skills and progresses to suck feeding. In some cases, this progress is seen throughout the stay on the unit but for some infants, particularly those with early feeding difficulties, establishing suck feeding continues post-discharge.11 The development of skills that contribute to successful suck feeding begin at birth with the promotion of a close and loving relationship involving communication between a caregiver and the infant.12 Support should be given to parents when deciding on a feeding method, whether breast or bottle, or a combination of both. In those cases where breastfeeding is chosen, provision of breast milk is prioritised and once suck feeding begins, support should be given to aid transition from tube feeding to breastfeeding.13,14 Before suck feeding begins, an infant might benefit from oral care with EBM or drops of EBM for pain management.15 This not only keeps the mouth in a healthy condition, improves comfort and decreases the risk of infection but also gives the infant its first taste of milk and supports early sensory development of taste and smell. Non-nutritive sucking can be introduced to encourage sucking for later feeds, and for soothing and regulation.16
These are some examples of specific SLT input on the NNU. It is worth mentioning that the focus of this article is on feeding, but SLT plays an important role in communication development in infants while on the NNU – early communication input is important because preterm infants are at high risk of communication difficulties that can persist into the school years.17
Suck feeding and respiratory support
The need for respiratory support can influence the decision to introduce suck feeds. Offering infants feeds while they are receiving non-invasive respiratory support is a controversial topic, with current guidelines suggesting careful consideration and multidisciplinary team (MDT) discussion.18 When introducing suck feeds in this cohort, it is vital to have SLT support, alongside consultation with the wider MDT to ensure successful outcomes.18 Prolonged need for respiratory support can increase the time it takes to achieve full suck feeding.
Research on feeding outcomes in neonates
Having normative data for the feeding journey of cohorts of infants distributed by gestational age will provide valuable information that can be used to inform parents of possible feeding outcomes and timelines. The feeding outcomes of neonates are discussed in various papers:
Majoli et al (2021)4 discuss oral feeding in relation to gestational age and note that the PMA at which oral feeding was introduced significantly impacts the time to reach full oral feeds. The authors state: ‘[It] may be important to focus on a specific targeted intervention, such as oral tactile stimulation, to strengthen the baby orally and therefore to facilitate the development of oral skills’, however they have no data to indicate this was used as a strategy.
Hoogewerf et al (2017)19 note a high prevalence of feeding difficulties in neonatal intensive care unit graduates at one and two years of age, finding that prolonged (<30 days) tube feeding and being born small for age are major risk factors. The authors mention the feeding scale with which infants were assessed but make no mention of SLT involvement in assessment or management.
Jackson et al (2016)7 look at predictors of time to achieve oral feeds in a late preterm cohort and note that PMA at the start of oral feeds and medical conditions affect the time taken to achieve full oral feeding. The authors mention feeding therapists on some units included in the study, however there is no specific data on their involvement.
Harding et al (2023)6 show that intervention from an SLT significantly quickens the acquisition of oral feeds but no specific details of the kinds of interventions performed to support feeding were mentioned in the data. The authors conclude that SLT plays a role in assessment of oral feeding readiness and supporting the journey to suck feeding, particularly in medically complex infants. With greater exploration of specific interventions and their direct impact, the role of SLT could be further valued.
Embedding SLT services into neonatal care
SLT complements medical and nursing expertise and an ideal model of care is to have SLT involvement in all infants’ feeding journeys. However, in an NNU with no funded SLT time, only the most complex infants are referred for feeding support.6 These infants most frequently fall into the extremely preterm infant group or the complex term group. This is in line with data from Harding et al,6 where the highest SLT support was within the extremely preterm infant group (35%; n=150) and the term group (28.5%; n=150). In these data, there was limited SLT involvement in other groups, who might be considered to fall into a lower risk category (17% in the very preterm and 8% in the mid-to-late preterm groups). This reflects the realities of a non-funded SLT service on an NNU.
An ideal model of care (FIGURE 1) would consist of specialised care plans for complex infants, targeted programmes (such as screening of high-risk groups) and implementation of universal principles for all infants (such as developmental care and family-integrated care, which aim to promote a set of principles to improve the lives of babies and their families on the unit).21 With an embedded SLT service on the NNU, all three tiers of this model of care could be implemented yielding better outcomes for infants and their families.
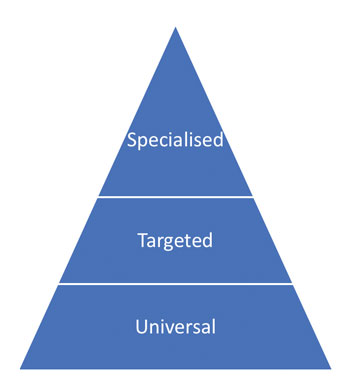
FIGURE 1 The levels of AHP care that should be present on all NNUs.20
Neonatal care is moving towards embedding AHP services in NNUs and each neonatal operational delivery network in England now has an established AHP team, consisting of SLTs, dietetics, occupational therapy, physiotherapy and psychology.22 Future research should focus on producing data on specific interventions. This will provide valuable information to drive forward the provision of SLT services on all units. The main purpose of this article was to focus on feeding problems and necessary support, but the role of the SLT in communication support is also vital and should be included in all service provision needs analyses.23
Conclusion
The act of feeding an infant is highly emotional for parents as it involves much more than just providing nutrition – this act is intrinsic in providing nourishment, nurturing, bonding and love. Meeting feeding milestones signifies great success for parents as it often coincides with the infant’s discharge home. Having a timeline to work towards may provide a sense of purpose for parents, more positive engagement in the feeding journey and better outcomes for the infant.
An infant should have SLT input throughout their neonatal stay, with feeding intervention starting in the pre-feeding stages and continuing throughout the journey of suck feeding. This is best achieved with an embedded SLT service. Normative data on the timeline of an infant’s feeding journey has the potential to help inform the length of time that inten-sive one-to-one SLT intervention is needed. This information should raise awareness of further data needed to inform staffing guidelines for SLTs on neonatal units.
Or read this article in our
Tablet/iPad edition
- Many infants receiving care on a neonatal unit will have feeding difficulties.
- Specialist assessment and intervention from a SLT can improve feeding outcomes.
- Data showing the outcomes of specific SLT intervention are limited.
- Having normative data for infants’ feeding journeys distributed by gestational age, will provide valuable information for advising parents of possible feeding timelines and inform staffing guidelines for SLTs.
Also published in Infant:


