Improving the effectiveness of aEEG monitoring: a novel CFM observation chart and a care bundle approach
Cerebral function monitoring (CFM) has become standard practice in monitoring infants with suspected encephalopathy in the UK, yet there are no standard recommendations of practice to ensure that continuous amplitude-integrated electroencephalography (aEEG) is as regularly monitored as other parameters in the neonatal intensive care setting. In this article, we present a simple intervention combining human factor principles and quality improvement (QI) methods to ensure regular timely review and documentation to improve the effectiveness of aEEG monitoring with a clear process of escalating concerns.
Helen Doyle
Advanced Neonatal Nurse Practitioner
Bharat Vakharia
Neonatal Consultant
Claudia Chetcuti Ganado
Neonatal Consultant
claudia.chetcutiganado@ldh.nhs.uk
Doyle H., Vakharia B., Chetcuti Ganado C. Improving the effectiveness of aEEG monitoring: a novel CFM observation chart and a care bundle approach. Infant 2023; 19(4): 127-32.
Background
The use of amplitude-integrated electroencephalography (aEEG)/ cerebral function monitoring (CFM) has become standard practice in the UK and the developed world for evaluating brain function in infants with suspected encephalopathy, usually as an adjunct to treatment with therapeutic hypothermia.1 Originally used in the 1960s to contin-uously monitor the brain activity of unconscious post-cardiac arrest adults, continuous aEEG technology was introduced to neonatal care in the 1980s primarily to monitor the brain function of sick neonates and subsequently as a tool to help guide selection for neuroprotective strategies.2,3 Since its early introduction to neonatal care, aEEG use has evolved significantly, and in the current day extends to monitoring infants with hypoxic ischaemia, intracranial haemorrhage, stroke, cardiac dysfunction, metabolic disorders, encephalopathy, suspected seizures and, in more recent years, to monitor the brain activity of the preterm population.4,5
The use of aEEG to detect seizures holds significant clinical value in the neonatal period. Seizures are more common in the neonatal period, particularly in the first week from birth, and are often the first sign of neurological dysfunction.6 Rates of neonatal seizures are estimated at 1-5 per 1,000 live births and their aetiology is often associated with serious underlying brain injury, such as hypoxic ischaemic encephalopathy (HIE), haemorrhage or stroke.7
Despite this prevalence in the newborn period, detection of seizures in neonates can be particularly difficult as their clinical manifestation is often subtle or entirely absent. Approximately 50-80% of seizures are estimated to go undetected where reliance is placed on clinical observation alone.8 Even among trained observers, clinical seizures are difficult to recognise and differentiate from normal neonatal behaviour. Autonomic signs of seizure activity such as episodes of apnoea, tachycardia, bradycardia and changes in blood pressure are often attributed to other causes such as sepsis or prematurity, conditions which are common in the neonatal intensive care unit (NICU).9 Consequently, the detection, treatment, and investigation of seizures in neonates without aEEG can be missed or delayed, further increasing damage to the neonatal brain leading to adverse neurodevelopment and subsequent behavioural, developmental and cognitive complications in later life.10
The problem
Within our tertiary level NICU, approx-imately 50-70 babies per year have monitoring of their brain wave activity using aEEG. Used primarily throughout cooling therapy, aEEG offers clinicians information about background cerebral activity, facilitates the detection of seizures and aids the prediction of neuro-developmental outcomes for term and preterm infants.11 Review of the aEEG trace occurs by the medical team primarily at ward rounds or handovers. Despite having aEEG reporting forms, documentation of aEEG findings is ad hoc and largely dependent on individual practices. The nursing team have no clear guidance when to escalate concerns and this has sometimes led to a significant delay in aEEG seizure recognition.
The rationale
Rennie et al12 identified that the aEEG is primarily used by clinicians who have minimal or no training in aEEG analysis and it is recognised that standardised training for nurses and doctors remains limited. However, as it is the bedside nurse who provides the continuous care and assessment of these babies, their role in the identification of aEEG changes is critical as they need to be able to recognise the need for timely escalation to the medical team.13,14
Lavery and Randall15 suggest that assessment of aEEG only takes a small amount of training in basic pattern recognition skills, and that nurses are particularly skilled in this as they constantly review incoming data, such as electrocardiogram (ECG) information and ventilator loops. Foreman and Thorngate16 agree, recognising that the bedside nurse is in the ideal position to identify behavioural and aEEG changes; they suggest that pattern recognition can be taught in a simple format allowing nurses to attain the skills for successful application and interpretation of aEEG.
Training provided to the local nursing team to date comes generally from colleagues and mentors throughout completion of their qualified in specialty (QIS) intensive care training, although this may be from staff who themselves have received minimal training. Ad hoc sessions are delivered at medical teaching or by company representatives and, where possible, the consultant team deliver bedside teaching sessions. However, attendance at these sessions is often workload and shift dependent. Thus, in practice, it appears that the surveillance and inter-pretation of aEEG is generally deemed to be a medical responsibility, despite the bedside nurse being the predominant caregiver for the baby and ideally placed to support this clinical need.
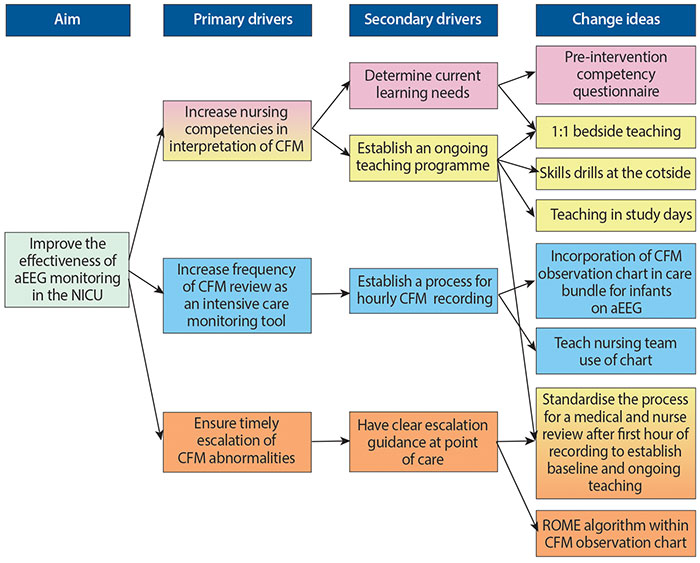
FIGURE 1 The project driver diagram.
Methodology
The aim of our project was to improve the effectiveness of aEEG monitoring on the neonatal unit. Using QI methodology, we designed a project that included a teaching package for nurses caring for infants on aEEG monitoring, a competency assessment, a novel CFM observation chart, a care bundle approach to monitoring aEEG hourly and a clear process of escalating concerns to the medical team.
Our primary drivers were (FIGURE 1):
- To increase nursing competencies in interpretation and escalation.
- To improve the frequency of CFM and documentation of findings.
- Ensure timely escalation of CFM abnormalities to the medical teams.
Phase 1: understanding the current level of competence
As a first step, it was important to understand the current level of competence among nurses caring for infants on aEEG monitoring. Staff were invited to complete an anonymised pre-training questionnaire. This served two purposes:
- To identify the level of competency and learning needs.
- To serve as a comparator measure once the teaching package was delivered.
Thirty QIS staff (approximately half of our unit QIS staff) were identified in the project proposal with a plan for continuing education outside of the project time frame. This was deemed an achievable number to support the project taking into consideration staff absences (sickness/ maternity leave/leaving post) and the time it would take to deliver the training.
Phase 2: Increasing the nursing competencies in CFM interpretation
The original aim was to teach at the QIS study days to reach staff who would primarily be providing care to those babies who may require aEEG. However, with the onset of COVID-19, all group meetings were discontinued due to social distancing regulations and nationally recognised challenges, including increased staff sickness and patient demand, meant training was more difficult than anticipated. Instead, teaching was held in small groups on a day-to-day basis. In practice, whenever there was an opportunity, staff were invited to bedside teaching about aEEG monitoring in neonates and given the option to participate in the service improvement project.
Improving the frequency of aEEG monitoring and documentation
To achieve this, the project team created a specific aEEG monitoring chart (FIGURE 2). The chart records the upper and lower margins of the aEEG to be plotted and colour coded. Red-amber-green ‘traffic light’ rated parameters support the identification of changes in aEEG pattern, which prompts escalation to senior medical review. The chart prompts the nursing team to review the aEEG hourly for evidence of electrical seizure activity and record the impedance in that time-frame. This ensures that each hour the impedance levels are assessed to be at a minimal level and the trace is a true and accurate representation of the neonatal brain activity and not electrical interference, which can lead to misleading information in aEEG pattern interpretation.5,11,13
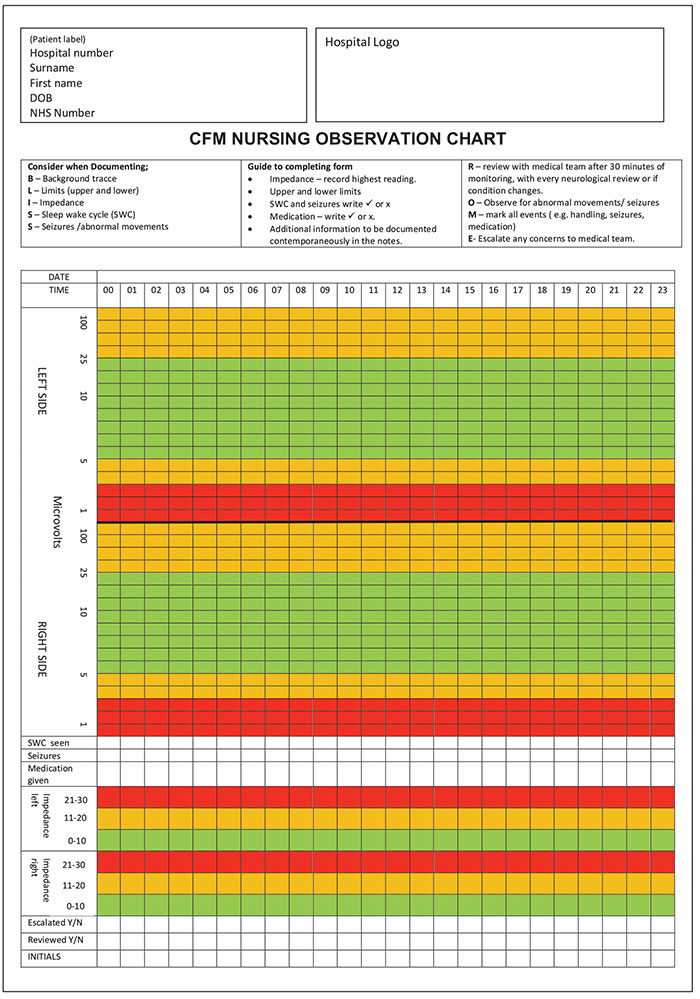
FIGURE 2 The aEEG monitoring chart.
Prompt escalation and timely review: the ROME algorithm
We created the mnemonic ROME to facilitate consolidating the process in practice. Using the human factor principle of a cognitive aid to support decision making, while embedding the correct process at the point of care, the mnemonic also helps to facilitate consolidation of the practice. The aEEG observation chart takes the nurse caring for a baby through the ROME care bundle. ROME stands for:
- Record the aEEG observations hourly
- Observe the baby for any abnormal movements in that hour
- Mark any events occurring
- Escalate concerns to the medical team.
The standard operating process was for the medical and nursing members to review the trace jointly 30 mins after starting the aEEG monitoring. This had the dual aim of improving the nursing competency in aEEG interpretation and serving as a baseline for the medical and nursing team. The nursing team was asked to escalate any limits within the amber and red zones or any changes to the baseline in that period.
Results
In total, 62 QIS staff were eligible for training. The teaching period ran from April to September 2020 and during this time 42 staff received the targeted aEEG training. Only 40 returned their pre-teaching questionnaire. Despite all 40 attending the targeted aEEG training, only 31 returned their post-teaching questionnaire (TABLE 1). Of these, two nursing members had not returned their pre-teaching paperwork, so this left 29 staff who completed both pre- and post-data, where paired analysis could be made.

TABLE 1 The post-teaching questionnaire.
45% of staff said they felt they cared for babies on CFM regularly, while 55% felt their exposure was infrequent. The ability for nursing staff to identify normal CFM parameters increased from 24% pre-implementation to 86% post-implementation (FIGURE 3). The confidence in their ability to recognise seizures increased from 35% to 76%.
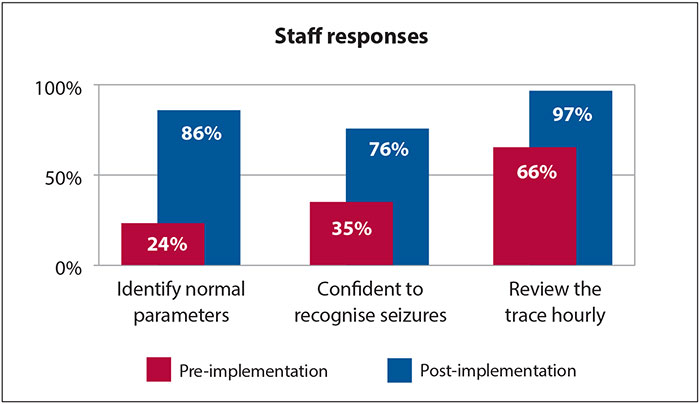
FIGURE 3 Graphical representation of the pre- and post-implementation responses to the project questionnaire (n=29).
Only 66% reviewed the trace hourly pre-implementation; this increased to 97% post-implementation. There were significant improvements to the nursing team’s ability to recognise aEEG traces and their terminology post-implementation (FIGURE 4).
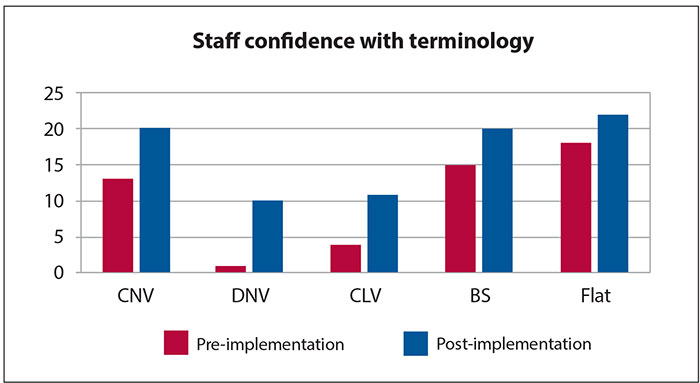
FIGURE 4 Nurses confidence with aEEG background terminology pre- and post-intervention. Key: CNV=continuous normal voltage; DNV=discontinuous normal voltage; CLV=continuous low voltage; BS=burst suppression.
Feedback from staff during this time was very positive, with decreased anxiety and a willingness to learn. The use of the new aEEG chart fully supported this process as it offers a visual representation of normal and abnormal and requires frequent use, which builds staff confidence.
Discussion
In clinical practice there are no set criteria for how often the aEEG trace should be reviewed. Our network guideline suggests the attending clinician should provide written documentation about the aEEG findings at 6, 24 and 48 hours and after rewarming.17 An online network infor-mation source (BEBOP)18 suggests the trace should be reviewed at every ward round while the nurse looking after the baby should document the aEEG in the patient notes at least once per shift. With the introduction of the new aEEG chart, we have ensured hourly review of the trace, specifically looking for seizures and checking for impedance; its completion provides documented evidence of regular review. Utilising this new resource, 100% of babies with aEEG now have documented evidence that their aEEG has been reviewed hourly.
Our post-implementation questionnaire findings demonstrated improvement in all areas of nursing competency (FIGURE 5).
By using a questionnaire with both closed and Likert-scaled questions, it was felt that enough information would be gained to form a basis of current team knowledge. While our initial sample size ambition was to reach all staff who might care for a baby on aEEG, it was recognised this was not achievable within the project timeframes and so a target of 30 QIS staff (approximately half of our unit QIS staff) was identified in the project proposal. Alongside the questionnaire, staff were introduced to the service improvement aims and methodology.
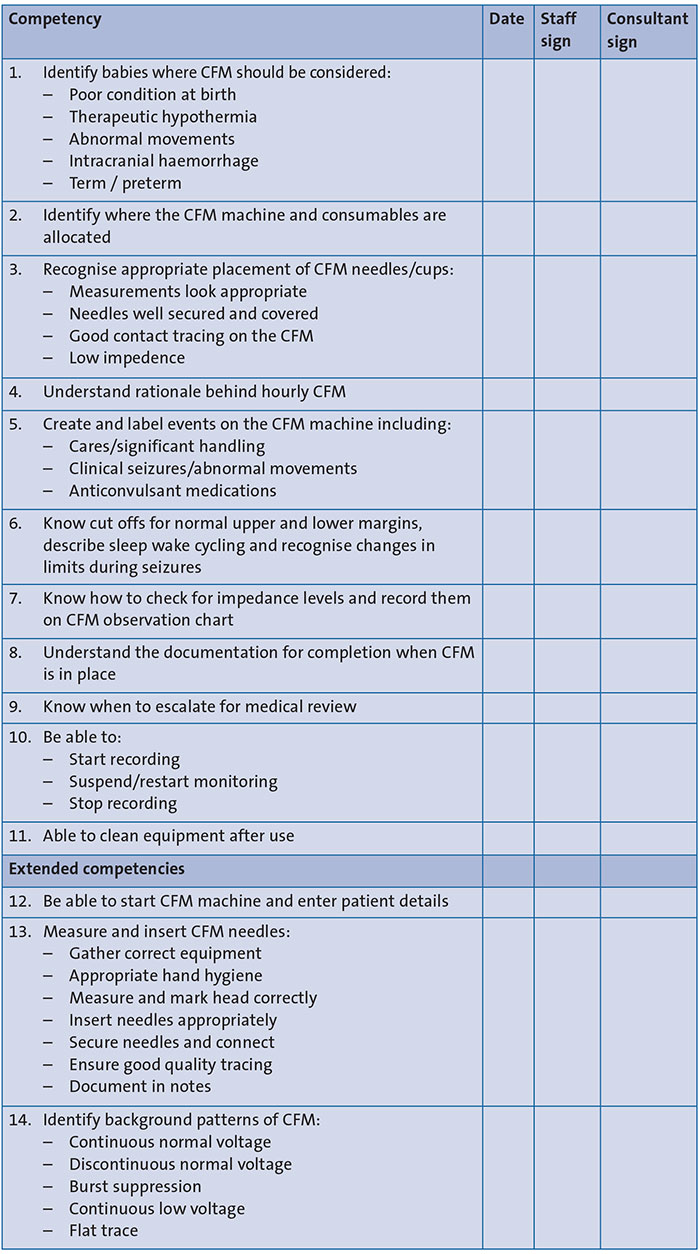
FIGURE 5 The CFM competency chart.
This project was met favourably by all team members, some of whom expressed anxiety at being allocated a patient on aEEG as they did not feel confident with the technology and information it offers, while others highlighted their anxiety around missing a seizure. Some also expressed concern about being unable to answer parent questions. This issue is particularly important in NICU as parents who are separated from their infants generally experience high levels of stress and anxiety; parental satisfaction is often reliant on their confidence and trust in the neonatal nurse charged with the care of their baby.19 In addition, staff anxiety compounded by a lack of clinical support can significantly contribute to staff sickness and retention so increased clinical confidence is key to maintaining a strong workforce.20
The COVID pandemic prevented capturing a large audience in study days so most of the teaching had to be carried out opportunistically at the bedside. While this added a considerable time element to the project, it afforded the project team more insight into current staff knowledge, which helped target the teaching content. Small group teaching is recognised to be more focused and interactive than large group teaching and enables discussion on complex topics.21
The aim of the project was to decrease time to detect seizures via increased knowledge and frequency of trace review. However, at the end of this project during the PDSA (plan, do, study, act) cycle, it was recognised that getting staff more familiar with the terminology could be a further enhancement and provided the drive behind an aEEG resource file that was subsequently put in place and is available for staff to consolidate their new learning.
Babies on aEEG in our NICU now have their trace reviewed and plotted hourly and any change in pattern, evidence of seizures or impedance problems are rapidly escalated. We have achieved a 100% engagement from the process and this has also been adopted by other network hospitals. Direct feedback from staff has identified the new chart as a useful tool to support clinical practice and staff education; its presence not only supports our documentation requirements but also facilitates bedside teaching by the medical team on their review of the trace.
In principle, 100% engagement in this process should improve the time to seizure detection and will avoid incidents where seizures are unrecognised for a prolonged period of time. We were unable to demon-strate this in the project timeframe and this is the major limitation of our project.
Conclusion
What was already known on the topic:
- aEEG monitoring has become standard practice in monitoring infants with suspected encephalopathy.
- Despite its widespread use there are no standardised guidelines to monitor and record aEEG at the bedside leading to the potential for delayed recognition of seizures.
What this study adds:
- Using simple quality improvement and human factor methodologies we ensured that aEEG is reviewed and recorded hourly by our nursing team.
- We propose a novel aEEG observation chart.
- We propose a care bundle approach to the monitoring of infants on aEEG to maximise the effectiveness of aEEG monitoring in practice.
Utilising a teaching and competency package coupled with a mnemonic care bundle approach to aEEG monitoring and a novel aEEG observation chart, we have ensured:
- hourly review and documentation of aEEG
- a process for timely escalation to the medical team
- a confident and empowered nursing workforce that recognises the concept of aEEG as an observation tool similar to intensive care monitoring of other observations, such as heart rate or temperature.
Ethical considerations
Ethics approval was sought prior to commencement of the project via ERGO II (Submission 56216). Staff participation in the study was entirely voluntary, and data obtained were anonymised to protect participant rights. In addition, gateway authority was sought from the local trust as a prerequisite to project commencement. As per the ERGO submission, all staff were informed that the questionnaire formed the basis of a service improvement project. Staff were given the option to access the training without having to participate in the project and informed completion of the pre-teaching questionnaire would be classed as participation consent. All staff who received the training were happy to complete the pre-questionnaire and offered verbal consent for their information to be used.
Acknowledgement
The authors would like to thank the nursing and medical team at the Luton and Dunstable Neonatal Unit for supporting this project and the East of England Operational Delivery Network in adopting this practice. Special thanks to Wendy Rogers, East of England Neuroprotection Nurse Lead, and Trina Valdez, Practice Development Nurse at Peterborough City Hospital for the adaptations on the CFM chart and making it a network document.
Or read this article in our
Tablet/iPad edition
- Despite widespread use, there are no standardised guidelines to monitor and record aEEG at the bedside, leading to potential for delayed recognition of neonatal seizures.
- We propose a novel aEEG observation chart and a care bundle approach to the monitoring of infants on aEEG.
- Using simple QI and human factor methodologies, we ensure that aEEG is reviewed and recorded hourly.
Also published in Infant:


