Navigating between technological and relational practice in neonatal care
As innovations in neonatal practice require clinicians to engage with increasingly technological medicine, staff must also prioritise family-integrated and relationship-centred care. These two modes of practice can compete for clinicians’ psychological resources. In this article I explore the implications of this dilemma and identify some ideas that might be useful in navigating the intersection of technological and relational practice.
Davy Evans
Clinical Psychologist
Birmingham Women’s and Children’s NHS Foundation Trust
davy.evans@nhs.net
I recently attended a perinatal medicine conference – the British Association of Perinatal Medicine (BAPM) Spring Conference in Birmingham, UK. As a clinical psychologist working in neonatal care, I found the programme’s wide-ranging focus extremely engaging. Within the space of 10 minutes, I heard discussions ranging from the use of artificial intelligence-controlled ventilation strategies to the devastating impact of perinatal trauma on parent-infant relationships. For me, these prompted reflections on a dilemma at the core of neonatal care:
How can clinicians practise such advanced, complex, hi-tech medicine in the same moment as being attuned to the significant emotional and relational needs of the babies and families they care for?
In this article I explore this dilemma and identify some ideas that might be useful in navigating this intersection between technological and relational practice.
The dilemma
Technological innovation has been at the heart of the field of neonatology in well-resourced countries since its emergence in the 19th century. The delivery room and neonatal unit continue to become more hi-tech environments filled with equipment and procedures that require extensive training and technical expertise (FIGURE 1).1 Increasingly, technologies such as newborn pulse oximetry screening are becoming standard practice in neonatal care and there are emerging technologies that aim to use algorithm-based machine-learning to improve the accuracy and responsiveness of a range of diagnostic, monitoring and treatment methods in the care of preterm and sick babies.2 To engage with this technology, critical care clinicians must deploy a range of complex cognitive skills underpinned by their executive functioning.3
Neonatal clinicians are required to learn and use advanced technologies while, at the same time, others in the field are advocating for the development of new and contrasting ways of working: family-integrated care (FiCare) and trauma-informed care (TiC). These models promote emotional attunement and a connection between clinicians and families through relationally responsive and sensitive practice. By means of collaborative involvement of families and integrating psychosocial support into standard care, initiatives such as FiCare and TiC aim to improve babies’ outcomes by empowering and enabling parents to buffer the toxic stress of preterm birth and hospital admission.4 These ways of working require neonatal clinicians to prioritise a completely different skill set:
- emotional intelligence5
- empathy6
- affective coregulation.4
Van Manen wrote of the neonatal context, that: “The health care provider… is not just a technician, but rather a careful, caring professional. As technology becomes more pervasive and perhaps more transparent, it is crucial for practitioners to gain a renewed understanding of how parents experience being with their children in the medical lifeworld.”7
Listening to the presentations at the BAPM conference, I felt acutely aware of the challenge facing practitioners who are required to engage with both of these ways of being: both technologically and relationally competent.
Although the cognitive, executive skills and emotional, social skills underpinning these two modes of practice rely on distinct abilities underpinned by separate brain networks and structures,8,9 they are by no means mutually exclusive or incompatible. Evidence suggests, however, that these processes can interfere with each other. The very process of switching between tasks increases cognitive load for medical staff,10 and is especially disruptive when switching between tasks with and without an emotional component.11 There is competition for a clinician’s psycho-logical resources between technological and relational practice.
Evidence from research into parental experience of neonatal care further illustrates the challenges of reconciling one’s relational presence with the technologised environment of the neonatal intensive care unit (NICU). With parents’ attunement to their baby’s cues so crucial for sensitive caregiving, parents report that the technological environment alienates them from their baby and their own parenting role.12 Van Manen writes about how technology as familiar as cardio-respiratory monitors can ‘mediate’ parents’ experience of and relationship with their baby, creating disconnection.7 ‘Mediate’ is used here in its phenomenological rather than its statistical sense: a baby becomes experienced through the monitors, rather than directly as a whole person. It seems reasonable to assume that a similar process of disconnection through technology-mediated relationships might occur for clinicians also.
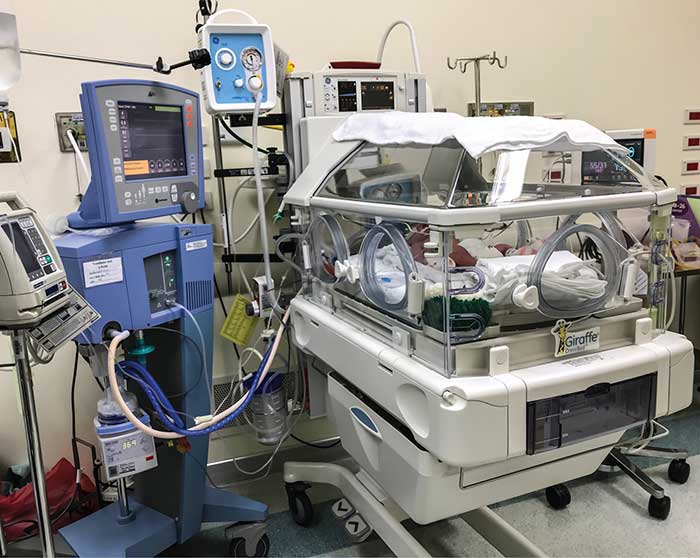
FIGURE 1 The hi-tech environment of the NICU presents clinicians with a dilemma between technological and relational practice.
The impact
One might wonder what relevance this dilemma has for the real world. This thought did occur to me, as I reflected on my experiences with my own clinical colleagues, many of whom are extremely skilled in both the technical and relational aspects of their work. However, this dialectic in neonatal practice does impact with real-life consequences. The switching between these modes described previously increases cognitive load, which has been shown to impair attuned communication.13
In conditions of high cognitive load, clinicians make poorer decisions and provide care that is more likely to be influenced by implicit stereotypes, which risks amplifying disparities in care and perpetuating health inequalities.14
Furthermore, this dilemma may result in stress and burnout for clinical staff. For example, Tawfik et al,15 reported that clinician burnout was more prevalent in NICUs that deployed technology such as digital health records. Mills and Cortezzo16 cite advances in neonatal medical technology as a significant source of moral distress for clinicians, as the ability to intervene earlier and more intensively brings competing values of ‘doing everything possible’ and ‘reducing suffering’ into greater conflict. Indeed, interviews with neonatal staff have revealed that clinicians are: “Reluctant to describe the NICU infant experience as traumatic. Hesitations relate to clinicians’ personal concerns that they may be seen as agents of trauma.”17
In other words, finding ways to reconcile these competing modes of practice is important for protecting babies, families and professionals.
Navigating the dilemma
To summarise the dilemma: neonatal care is simultaneously becoming increasingly technologised and increasingly relational in ways that can compete for the foreground of clinicians’ practice. Such competition might have harmful implications for babies, families and staff. It is important to acknowledge that the system is being required to continually improve in both aspects of practice in the interest of reducing mortality and improving short- and long-term outcomes for babies and families.18 In the following sections, I will explore the value in different approaches to responding to this dilemma.
Specialising and separating roles
Anecdotally, one attempt to ‘resolve’ the dilemma between technological and relational practice is to assign these different roles separately to different members of the clinical team. This is an attempted solution I have witnessed in many healthcare contexts far beyond neonatal care. In fact, individual differences might well mean that some clinicians may feel better suited for compassionate, empathic communication while others may feel more adept at the technical, systematic aspects of the work. However, such artificial boundaries are not realistic or workable in practice. In order to fully appreciate and comprehend families’ and colleagues’ experience in my work I must grasp some of the technical aspects of the context. Similarly, psycho-logical skills must be shared across the whole team in order for families to feel safe and cared for, and for a service to take a truly trauma-informed approach. So, delegation of these modes of practice is not a workable solution.
Driving improvements
Another common response to the dilemma is to try and get better at both skill sets. Practice in both modes might well help clinicians embed the required skills to the point that they become more automatic and less controlled (and therefore less effortful). Staff-focused training and education can improve a clinician’s skills in empathic communication,19 and guidelines have been written for the most effective means of delivering this education.20
In the realm of technical proficiency, there is a significant move towards ‘optimising performance and reducing errors’ particularly through optimising human factors.1 Much of this ‘human factors optimising’, however, comes down to reducing human error (eg through decision support tools; reducing cognitive load), rather than valuing and harnessing our uniquely human relational qualities, which further alienates clinicians from their relational practice.
Sitting with the dilemma
Simply fractioning off or getting better at each element of the technological/relational dialectic will not imminently resolve the conflict. My view is that, before we can reconcile these modes, we must first accept that both must co-exist, that this will lead to some tension, and that the task at hand is about finding signposts, way-markers and a compass to help us navigate between these domains in the landscape of neonatal practice.
In my experience, it is most helpful to start by taking the time to notice in which mode you are currently operating: to slow down and reflectively attend to what you are currently doing. After all, how can you navigate towards something if you are not aware of where you currently are? Vittner21 described a range of reflective practices that can help us find coherence in new approaches to neonatal care, including guided dialogue, role-playing, journaling, and guided imagery. Structured reflective spaces, such as psychological pre- and debriefs are being used increasingly frequently in neonatal care22 as a means of supporting staff to manage the impact of their work.23 In a fascinating episode of the Being Better, Together podcast, Dr Hena Syed-Sabir, Clinical Psychologist at Paediatric Intensive Care at Birmingham Children’s Hospital, speaks about the value of psychological debrief in critical care.

FIGURE 1 To listen to Dr Hena Syed-Sabir's podcast scan the left QR code. To listen to Davy Evans’ podcast scan the right QR code.
Another practice that may assist clinicians in attending to their current mode, in readiness for potential transitions to other modes, is that of mindfulness. Mindfulness describes the practice of focusing one’s attention on present-moment experience, with a non-judgemental attitude: it is a way of attuning to one’s own emotional world. When enhanced through training and practice, mindfulness skills can reduce stress and burnout in healthcare staff.24
Despite the likely benefits of mindfulness practice in this context, I often encounter reluctance to engage with it. A common barrier I have noticed is the perceived time and effort required to cultivate a sufficiently frequent and focused mindfulness practice. One solution to this is the use of brief, momentary methods of ‘checking in’ and ‘rebooting’ using mindful awareness of one’s self. An example is the ‘internal weather report’. This exercise invites you to turn your attention inwards, to notice any sensations and feelings that you find within, and then to bring to mind weather imagery that symbolises how you feel in that moment. I have written else-where about how helpful this practice can be in navigating the transition between different modes of practice.25 For example, I encourage colleagues (and myself) to use the internal weather report at the start and end of shifts to aid in the transition from a work mode to an off-duty mode. Becoming aware of your internal weather can help you attend to what mode you are functioning in and what might need to change to allow you to shift into a different way of working. You can access a guided recording of this exercise that I made by scanning the QR code above. Although the recording focuses on navi-gating shift transitions, it could equally be applied to the shifts between other modes of practice, for instance the technological and the relational.
All of these approaches to managing the dilemma between technological and relational practice, from empathy-focused communication training and reflective debriefs to mindfulness exercises, can be facilitated by a clinical psychologist. In addition to providing direct clinical input to families in neonatal care, clinical psychologists can work with the wider team to support them to navigate the various challenges they encounter in their work.
Final thoughts
The wide-ranging focus of the BAPM conference programme was an explicit, deliberate attempt to educate and train the multidisciplinary neonatal team together, in a joined up way, as advocated for in the recent Ockenden review. The more this multidisciplinary approach is embedded in neonatal care, the more technological and relational practices will be integrated into a shared way of working. Both are crucial for improving the outcomes of babies and families. In this article I have shared some reflections on the consequences of this integration, and some ways to help staff to navigate the expanding territory of neonatal care, but more research is needed to understand clinicians’ experiences of this dilemma and the best ways to support them in their work.
Or read this article in our
Tablet/iPad edition
- Recent innovations in care present neonatal clinicians with a dilemma between technological and relational practice.
- These modes of practice can compete for clinicians’ psychological resources, impacting on quality and safety of care.
- Finding ways to reconcile and navigate these domains is important for protecting babies, families and healthcare professionals.
- Clinical psychologists are well placed to facilitate the proposed solutions.
Also published in Infant:


