Developing newly qualified nurses’ confidence within neonatal intensive care
Newly-registered nurses can struggle with the transition from student to practitioner; achieving competence within a critical care area, such as neonatal care, can be particularly challenging. Education is pivotal for nurturing new registrants so that they stay in their specialist area. A neonatal competency framework for new neonatal nurses in their first year of practice was implemented in South Wales. This article discusses the importance of supporting new nurses to develop their knowledge, skills, confidence and competence in neonatal care and why this is important for staff retention.
Jessica M. Beynon
Practice Development Lead
Neonatal Services
Singleton Hospital, Swansea Bay
Health Board
jessica.beynon@wales.nhs.uk
Background
Neonatal intensive care is a specialist critical care area falling between maternity and paediatric services, which attracts newly registered nurses from differing parts of the nursing register. As a practice development nurse based within a sub-regional neonatal intensive care setting, I developed a growing awareness that there was a significant ‘transition shock’1 experienced by newly registered nurses when they became registrants in their first post in neonatal services. The retention of these staff nurses caused great concern; retention of nurses is a ‘far greater challenge’ for the NHS than recruiting enough students for undergraduate training.2
Several studies3-5 have identified that newly registered nurses struggle with the transition from student to newly qualified nurse; this is recognised as a part of the journey from novice to expert.6 Yet there is a lack of evidence of how these new registrants adapt within specialist areas, namely neonatal services. I have had first-hand experience of working closely with newly registered staff and have seen how they experience mixed emotions while they aim to develop confidence and competence in their first professional role – the excitement of becoming a staff nurse combined with the trepidation of losing the security and protection of student status.
Neonatal care in Wales
The Wales Neonatal Network is made up of four health communities capable of delivering a range of care. Around 35,000 babies are born each year in Wales and 9-10% of these will need admission to a neonatal unit. There are 10 neonatal units in Wales providing a range of differ-ent levels of care. The changes to neonatal services were driven by the South Wales programme in 2013, which realigned the number of specialist jobs into a smaller more concentrated area aiming to centralise acute services within the neonatal specialty.
This, combined with the natural movement of staff through retirement and other forces, has meant that there has been a continued shortage of staff,7 which has led to vacancies being filled by a substantial number of newly registered staff nurses.
Role identification
Newly registered nursing staff are expected to practise safely and ensure the safe and professional delegation of care.8 It is challenging for them to learn how to do this while trying to align their respon-sibilities to the patients, parents, the wider nursing team and with the health boards and Nursing and Midwifery Council. The Nursing and Midwifery Council9 asks nurses to demonstrate knowledge and skills while caring for people of all ages and across all care settings, but how this is achieved is down to individual health boards and different specialist areas.
Competence of newly registered staff
Competence can be described as the combination of training, skills, experience and knowledge that a person has and their ability to apply this to perform a specific task. The term competency covers a complicated and extensive concept, which comprises many aspects of behaviour, core capabilities, technical expertise, and functional, management and organi-sational competencies. It includes qualities such as:
- performance
- attention to detail
- asking critical questions
- communication
- cooperation/teamwork
- delegation
- flexibility
- responsiveness
- reliability
- initiative
- judgement
- leadership
- problem solving
- commitment to safety
- quality control.
Achieving competence within a critical care area proves particularly challenging for the newly registered practitioner. There is an expectation that they will ‘hit the floor running’10 yet this role change – from graduate to registered nurse – involves a myriad of emotions. They have to deal with the many factors that comprise nursing in the 21st century: advanced duties, fast-paced service, personalised care, greater responsibility, new clinical opportunities, specialisation, quality enhancement, educating other staff members, research nursing and, importantly, the impact of medical technologies. Technology has reshaped the way nurses work and critical care is a highly technologically-based specialty. The role of education is pivotal for supporting and developing new registrants.
A solid education will provide the foundational skills needed to succeed but integration of learning into practice is vital in supporting newly registered staff to achieve competency. It is worth noting that the less confident the newly registered staff nurse feels, the more concerns they have in terms of their own competence and practice.11
Introduction to change
In 2016 a literature review revealed that there were a number of competency documents available throughout the neonatal network within Wales; however, each required something slightly different from new registrants. This, coupled with differing health board requirements for newly registered nurses’ preceptorship programmes, led to different skills being attained by the new registrants within neonatal services in South Wales. Competences of new registrants were assessed using a competency document and the recorded observations of staff nurses working alongside them – the staff nurse would observe and evaluate the knowledge and skills of the newly registered staff nurse in order to assess their level of competence.
The competency document that was used had not been reviewed for a number of years and required a tick box approach to defining competence with limited weight being placed on the document by both the new registrant and the existing staff group. A tick box can assess technical skills, however, it does little to tell you about the newly qualified practitioner’s ability to deliver care on a practical basis.12
Building foundations on stone not sand
Although there were a number of competency documents available through-out the Welsh neonatal network, the All-Wales Neonatal Nurse Education Network felt that they did not reflect the complexities of current practice. The original induction documents contained details of ward routine along with health and safety requirements, but there was little assessment of the clinical skills and knowledge of new registrants. In light of this and the need to retain new registrants recruited in a specialist area, the documents were reviewed and became one of the driving forces for change. The All-Wales Neonatal Nurse Education group collectively felt that competency documents provided a benchmark of the new registrant but having different documents clouded the assessment of newly registered nurses’ competence.
All of the documents in use within South Wales were collated and reviewed over a six-month period in 2016, as well as other UK documents. The decision was made to adapt the framework in line with both the Royal College of Nursing neonatal standards13 and the Nursing and Midwifery Council standards for competence.14 The group aimed to implement these standards across South Wales, which meant redefining and redesigning the competency framework so that all new registrants receive the same document regardless of the neonatal unit they begin their career in.
The new competency document provided comprehensive assessment of clinical skills and knowledge. For example, previous versions stated:
- Is familiar with neonatal documentation, ITU/HDU charts, monitoring charts, feed/fluid charts.
- Demonstration of ability to assess, plan, implement and evaluate care for neonatal fluid, electrolyte, nutrition and elimination management;
- Demonstration of ability to assess, plan, implement and evaluate care in neonatal thermoregulation management.
The new document requires:
The new All-Wales competency document was adapted for use within South Wales and was implemented for use in 2017, this was rolled out for all new registrants in South Wales within level 2 (local neonatal) and level 3 (neonatal intensive care) units.
Within Swansea this was complemented by classroom-based teaching sessions delivered by the practice development teams and neonatal consultants. This cemented the link between theory and practice. Clinical supervision sessions were held to ensure that the newly registered nurse developed peer support and emotional resilience. This helped the nurse to increase professional competence through a framework of learning. While this is not a new concept and other neonatal networks currently provide this framework and programme, this was the first time that this had been put into practice in Swansea.
The Swansea programme aimed to optimise the recruitment and retention of nurses into neonatal care. It was designed to provide a supportive learning environ-ment to facilitate the learning experience of staff with little or no previous neonatal experience. It provides a structured and comprehensive teaching programme delivered over a six-month period, one day a month, and has two main aims:
- To develop the theoretical knowledge and clinical skills to deliver safe and effective care that meets the unique physical, emotional and social needs of the preterm neonate and his/her family.
- To provide educational support and development for the newly registered nurse.
The Swansea programme was facilitated by clinical educators with significant experience within neonatal care. The clinical educators would combine theoretical, practical and skills-based knowledge to help the newly registered nurse. The programme was supported by the senior management team. Structured teaching time was dedicated within the first year of practice for newly registered staff nurses. Skills were developed by provision of themed study days (eg respiratory/cardiovascular and the deteriorating neonate) and a practice development nurse worked alongside the new registrant to assess skills (eg caring for babies on non-invasive respiratory support and aseptic non-touch technique practical assessments). The neonatal ward sisters aimed to maximise learning opportunities wherever possible.
New registrant days were introduced for all new staff nurses within neonatal services within South Wales. A yearly study day was introduced in order to facilitate peer relationships within the small specialist area of neonatal care. The study day had the objective of developing the skills and knowledge of new registrants and developing tools to assist with improving resilience levels in new staff.
There was an increased onus on the new registrants to undertake and complete their competency document as this provided the springboard for ‘qualified in specialty (QIS)’ modules and further role development (eg medicines’ management and neonatal life support courses). Within the document, there was an identified timescale with clear roles and responsibilities outlined.
A change in practice
TABLE 1 shows the number of new registrants employed into Swansea Bay Neonatal Services before and after the competency framework programme was introduced.
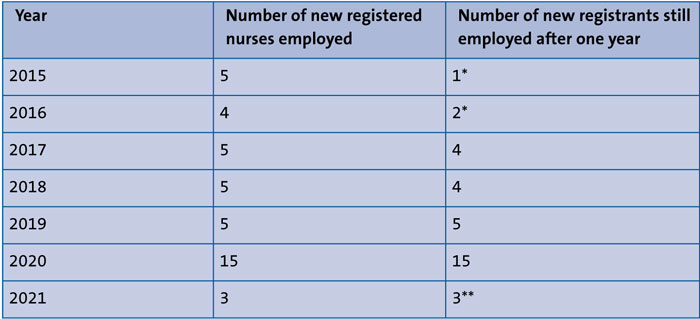
TABLE 1 The number of new registrants employed into Swansea Bay Neonatal Services. *Prior to the introduction of the competency framework programme. **At the end of 2021.
Prior to the introduction of the competency framework programme, staff exit interviews indicated that they were leaving because they felt overwhelmed with the changing role and expectations of a newly registered nurse.
The adoption of the competency framework with educational support aimed to reduce the attrition of new registrants within Swansea. At first this was a long-term aim but it became obvious in a short time (under two years) that keeping new registrants increased dramatically and the majority of new registrants were still employed within neonatal services after one year.
The new registrants developed their confidence and ability through the structured education programme, as assessed by an anonymous electronic survey that collected the thoughts of the new registrants via questions such as such as:
- How did you find working to the competency document?
- Were the study days useful?
- Were the clinical supervision sessions helpful?
Some of the comments included:
- “Really helpful and informative. Helped me to develop my knowledge.”
- “I was given opportunities and felt more confident in my practice.”
- “The neonatal study days gave me more confidence.”
The survey also highlighted areas where the new registrants felt they required further support and development,15 which led to them actively seeking out knowledge and skills from the other nurses in the neonatal team. One of the most interesting findings was that there was a reduction of clinical incidents that new registrants were involved in.
The All-Wales neonatal competency framework for newly registered neonatal nurses is designed for use within the first year of practice. 62% of the newly registered neonatal nurses completed the document within a six to nine month timescale and were keen to progress their own professional development.
Through direct observation, performance appraisals and development reviews, and by talking to staff about how they feel a year on from starting, it appears that there have been a number of challenges for the new registrants (eg COVID-19 and having to move training to an online platform), but their ability to hit the ground running has improved. It remains to be seen whether the results over the last two years can be replicated for the upcoming intakes.
Discussion
Retention of nurses in neonatal practice is a constant challenge that has a significant impact on patient care. In 2016, Bliss noted that neonatal units in Wales are under-staffed, with only two out of 10 neonatal units having enough nurses to staff all of their cots in line with national safety and quality standards. This echoed the findings from the Bliss report, Hanging in the Balance, which stated that two thirds of neonatal units did not have enough specialist nurses to meet British Association of Perinatal Medicine staffing guidance.16
Transition shock refers to the initial stage of role adaptation for newly graduated registered nurses. The new nurse often identifies their initial professional adjustment in terms of feelings of anxiety, insecurity, inadequacy and instability produced when facing their new role, responsibilities, relationships and their perceived lack of knowledge.1 Transition shock can be viewed as a rite of passage when adapting from student to staff nurse,17 however, support in the form of education can ease some of the stresses and help them to become safe competent nurses acting within professional standards.
The updated neonatal competency document delivers a robust assessment of competence within the clinical area but it was not without its problems. Some of the competencies were not as easily transferrable as first thought and the framework had to be altered to reflect changing professional guidance and standards.
The educational subgroup has had regular meetings based on new registrants’ thoughts to maintain a valid practical document and build on developing competence in newly registered nurses.
The competency framework and theoretical sessions pave the way for a seamless transition into the QIS modules available to neonatal nurses within South Wales by providing the solid foundations of knowledge that the QIS modules build upon.
Conclusion
The introduction of a neonatal compe-tency framework across South Wales has guided new registrants to progress their skills and knowledge within the first year of practice so as to become confident and competent as junior staff nurses. Fully supporting new registrants with education underpinning the link between theory and practice helps them to make the transition from student to staff nurse.
Staff retention is key to developing neonatal nurses for the future in line with national safety and quality standards. The formalised programme has assisted newly registered nurses to gain confidence and develop in their role. This has been achieved with the support and teaching of the wider neonatal team, which has been invaluable to the new staff nurses.
Or read this article in our
Tablet/iPad edition
- There was need to address common issues of ‘transition shock’ in new registrants within neonatal care.
- A common competency document was implemented across a number of neonatal units within South Wales
- Development of a programme for newly registered staff nurses improved their knowledge, skills, confidence and competence, and helped to retain staff.
Also published in Infant:


